When it comes to home or office design, often the smallest details make the biggest impact. We meticulously choose paint colors, furniture, and fixtures, but how often do we consider the humble HVAC grille? For too long, these essential components have been an afterthought, a functional necessity that detracts from an otherwise polished aesthetic.
But what if your grilles could be more than just functional? What if they could be a subtle design element, seamlessly blending with your decor or even becoming a quiet statement piece? That’s precisely the vision behind AirScape’s custom grilles, made in the U.S. right here in Medford, Oregon.
Beyond Basic: Why Go Custom with your Grilles?
Standard, off-the-shelf grilles are often generic, clunky, and limited in design. They rarely match your specific aesthetic and can stick out like a sore thumb. Custom grilles on the other hand, offer:
Seamless Integration – Match your grilles to your walls, ceilings, or even your flooring for a cohesive look.
Enhanced Aesthetics – Move beyond basic designs with unique patterns, materials, and finishes.
Perfect Fit – Customize your grille size by the eighth inch. No more struggling with ill-fitting grilles or unsightly gaps.
Quality Materials – 1/8” thick aluminum, 5mm GeoTone, 3mm Black Acrylic, or 1/4” Bamboo Ply, 16 gauge Galvanized Steel
Choosing Your AirScape Grille
AirScape custom grilles come in two primary types, each designed for a specific installation style:
Flat Grilles: The Modern, Low-Profile Look
Imagine a grille that lies perfectly flush with your surface, almost disappearing into the background. That’s the beauty of AirScape’s perforated flat grilles.
Design Philosophy – These grilles are designed to sit on the surface of your wall or ceiling. They don’t have a recessed portion that fits into the duct opening. The entire panel is visible, offering a sleek, contemporary aesthetic.
Precision Sizing – When you order a flat grille, the size you specify is the exact overall outer dimension of the grille itself. This is crucial for planning your installation and achieving that seamless look.
Design Perforated Flat Grilles Here
Flanged Grilles: The Secure, Finished Fit
For a more traditional and securely installed option that neatly frames your duct opening, AirScape offers perforated flanged grilles.
Design Philosophy – These grilles feature a flange, which is a border that overlaps the duct opening. The main body of the grille fits inside the opening, with the flange holding it securely against the wall or ceiling. This creates a neat, finished edge around the duct.
Installation Clarity – With flanged grilles, the LIST size refers to the size of the hole or duct opening you want the grille to fit into. The overall dimensions of the grille will be slightly larger.
Durable Construction – The flange grilles are made from 16 GA galvanized steel, built to last and suitable for a wide range of indoor and outdoor uses.
Ideal For – Any application where you need to cleanly cover and finish a duct opening. They provide a sturdy, professional appearance and are a popular choice for both residential and commercial projects.
Design your Perforated Flanged Grille Here
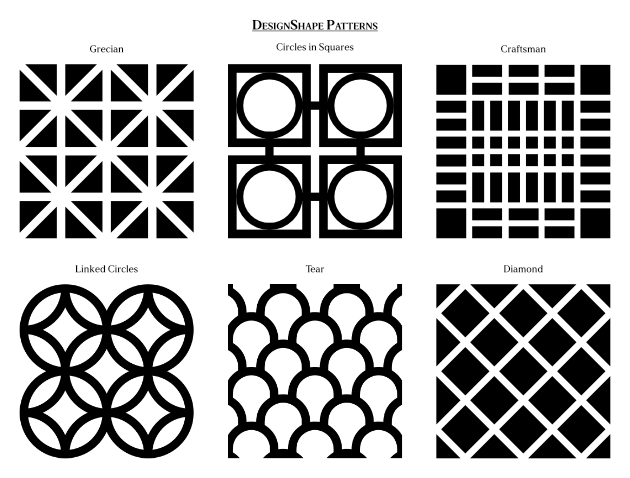
Unleash Your Inner Design with DesignShape
AirScape understands that every space is unique. That’s why every grille has a plethora of options that allow you to make your grilles how you want.
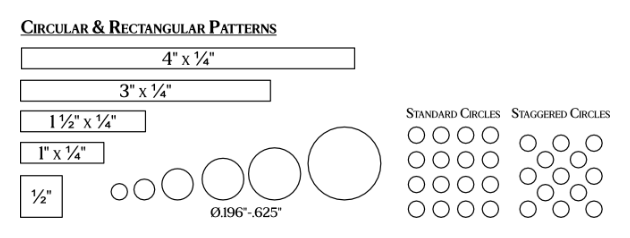
Size and Shape – From round grilles with 1/8″ diameter changes, and 1/4″ border changes, to rectangular grilles with 1/8″ changes for length and width, and 1/4″ changes to the border, provides over 1.5 million combinations between shape and size.
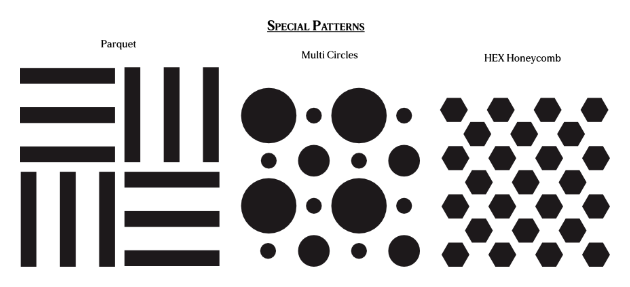
Patterns and Scaling – Perforated grilles made on the punch allow for 6 different patterns, with multiple sizing options for 3 of the patterns bringing to 11 different options to choose from. While the DesignShape grilles have 6 different patterns each, each pattern has several different pattern scaling and sizing options. This provides over 10 million options to choose from between the different patterns and scaling options.
Screw Holes – Specify the number and location of screw holes for a perfect, secure mounting.
Design your DesignShape Grille Here
The Process Behind our Grilles
Perforated Grilles
The secret to the precision and quality of our perforated flat and flanged grilles is a state-of-the-art Amada AE-2510 NT CNC turret punch press.
Punching Through Metal
The process begins with a digital design. Our engineer creates the specific pattern for the perforated grille using CAD (Computer Aided Design) software. The design is then translated into a program with machine-specific instructions for the AE-2510 NT. The program then tells the machine exactly where to place each punch, what type of punch to use, and in what order. Combined with a servo-electric drive, the AE-2510 NT is able to punch holes with incredible speed and precision in the metal.
Flange Bending
The HG-8025 Press Brake is a state-of-the-art CNC press brake. Its primary function is to precisely bend sheet metal into a variety of shapes, making it a key piece of equipment for producing products like the flanged grilles.
How it Bends Metal
A press brake works by using two sets of tools: an upper tool called a punch and a lower tool called a die. The CNC program tells the operator which tools are needed for the bend. The CNC uses a multi-axis backgauge to set the stop location that accurately places the metal at the exact location needed for each bend. The operator follows the step by step instructions shown on the monitor and when the metal is set in place, the operator uses the foot petal to activate the hydraulic system. The hydraulic system is activated, and the upper row of punches clamps down on the metal in place, this causes the metal to bend at the angles set by the die and punch.
DesignShape
The ShopSabre Pro 408 is a high-performance, industrial-grade CNC router. It’s designed for precision cutting, carving, and routing a wide variety of materials.
How DesignShape Grilles are Made
When the grille design is created, an engineer uses a CAD program to convert the design into g-code, the precise set of instructions that CNC machines read. The engineer places a sheet of the desired material on the router’s bed, loads the g-code, and the machine automatically cuts the grille to the exact design. From there the grille goes through a series of specialized finishing before it’s prepared for shipping.
The Difference of Customization
With a plethora of customization, create a unique grille that will seamlessly integrate into the aesthetics of your home. Imagine replacing those generic, off-white vents with a sleek, black acrylic flat grille that disappears into your dark ceiling, or a powder-coated aluminum flanged grille that perfectly matches your wall trim. The visual impact is immediate and significant.