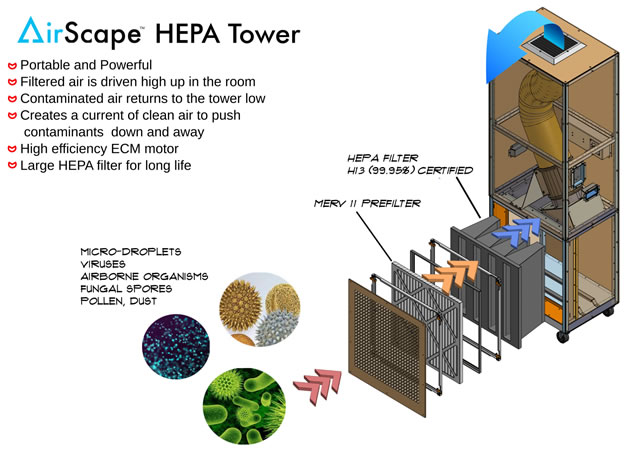
It is important to think about filtration, ventilation and air cleaning in order to mitigate risk of COVID-19 transmission.
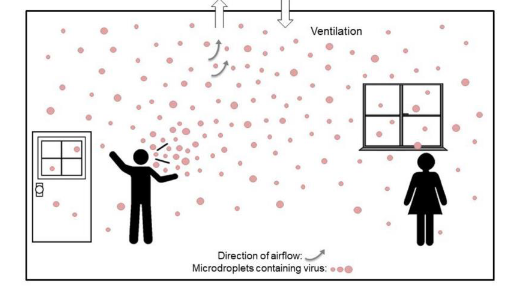
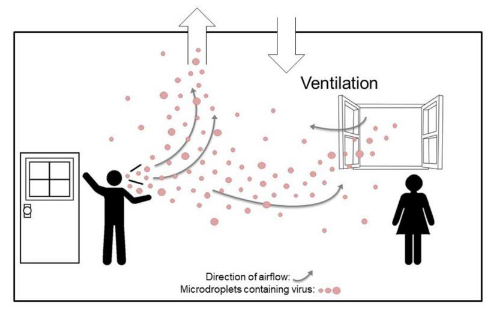
Let’s define some terms :
Droplets are propelled through the air, visible but fall to the ground after traveling 3-6 feet. Published research which has been replicated shows that droplets are only important when coughing and sneezing
Aerosols are much smaller than droplets (generally considered to be anywhere from 1 to 10 microns). They can be generated by talking, or by evaporation of droplets.
Aerosol (also referred to as “airborne”) transmission is similar to droplet transmission, except that the bits of fluid are so small that they can linger in the air for minutes up to 16 hours. Fears AC, Klimstra WB, Duprex P, et al. Comparative dynamic aerosol efficiencies of three emergent coronaviruses and the unusual persistence of SARS-CoV-2 in aerosol suspensions. medRxiv 2020:2020.04.13.20063784. doi: 10.1101/2020.04.13.20063784
https://www.sciencedirect.com/science/article/abs/pii/S0360132320302183
Appropriate air filtration and ventilation ensures that adequate dilution is achieved where and when needed, avoiding the build-up of viral contamination
Ventilation is the replacement of stale or noxious air with fresh air to a space or building by natural or mechanical means (ISO, 2017). It controls how quickly room air is removed and replaced over a period of time. Ventilation plays a critical role in removing exhaled virus-laden air, thus lowering the overall concentration and therefore any subsequent dose inhaled by the occupants.
HEPA is a type of pleated mechanical air filter. It is an acronym for “high efficiency particulate air [filter]” (as officially defined by the U.S. Dept. of Energy). This type of air filter can remove at least 99.97% of dust, pollen, mold, bacteria, and any airborne particles with a size of 0.3 microns (µm).
Public health messaging can be confusing. Scientists have issued a global statement through the World Health Organization stating that when it comes to COVID-19, the evidence overwhelmingly supports aerosol transmission.
With infectious diseases transmitted through aerosols, HVAC systems can have a major effect on the transmission from the primary host to secondary hosts. Decreasing exposure of secondary hosts is an important step in curtailing the spread of infectious diseases. HVAC systems impact the distribution and bio-burden of infectious aerosols.
https://www.ashrae.org/file%20library/about/position%20documents/pd_infectiousaerosols_2020.pdf
It is important to visualize the mechanism by which COVID-19 is transmitted, in order that individuals and institutions can understand how to protect themselves.
The closer you are to someone releasing virus-carrying aerosols, the more likely you are to breathe in larger amounts of virus. We know from detailed, rigorous studies that when individuals talk in close proximity, aerosols dominate transmission.
Superspreading events, where one person infects many, occur almost exclusively in indoor locations and are driving the pandemic. These observations are supported and explained by aerosols, and are very difficult or impossible to explain by droplets. https://www.medrxiv.org/content/10.1101/2020.02.28.20029272v2
Contact tracing shows that, when it comes to COVID-19, being outdoors is 20 times safer than being indoors, which argues that aerosol transmission is much more important than droplets. Outdoors, there’s plenty of air in which aerosols can become diluted; not so indoors.
As we move from warm weather outdoor activity season into autumn and winter indoor season, the Airscape HEPA.Tower provides an excellent ventilation solution to create fresh air indoors.